Oscar Health – revolutionizing health insurance through data analytics

A tech startup, powered by data analytics, is disrupting a massive industry through providing simpler and more affordable health insurance
Oscar Health was founded in 2013 as a company that aims to humanize healthcare driven by innovative technology, data and design delivered to customers in the simplest way possible. Within 18 months of launch, the company’s market share went from 0% to 15%. As of today, Oscar has attracted $700million+ in funding with $2.7Bn valuation.
Diving into a massive industry:
Oscar is trying to revolutionize a $3 trillion global healthcare industry, which in US alone, constitutes 20% of GDP and has a reputation for being challenging and inherently complex. We have often heard people complain “Health Insurance is the Worst” and why not! “It’s a wildly complicated business to be in,” says Segel, one of the co-founders of Oscar. “You have to deal with doctors, hospitals, pharmacies, banks, regulators — and it’s even more confusing for consumers.”
A simpler and more affordable product:
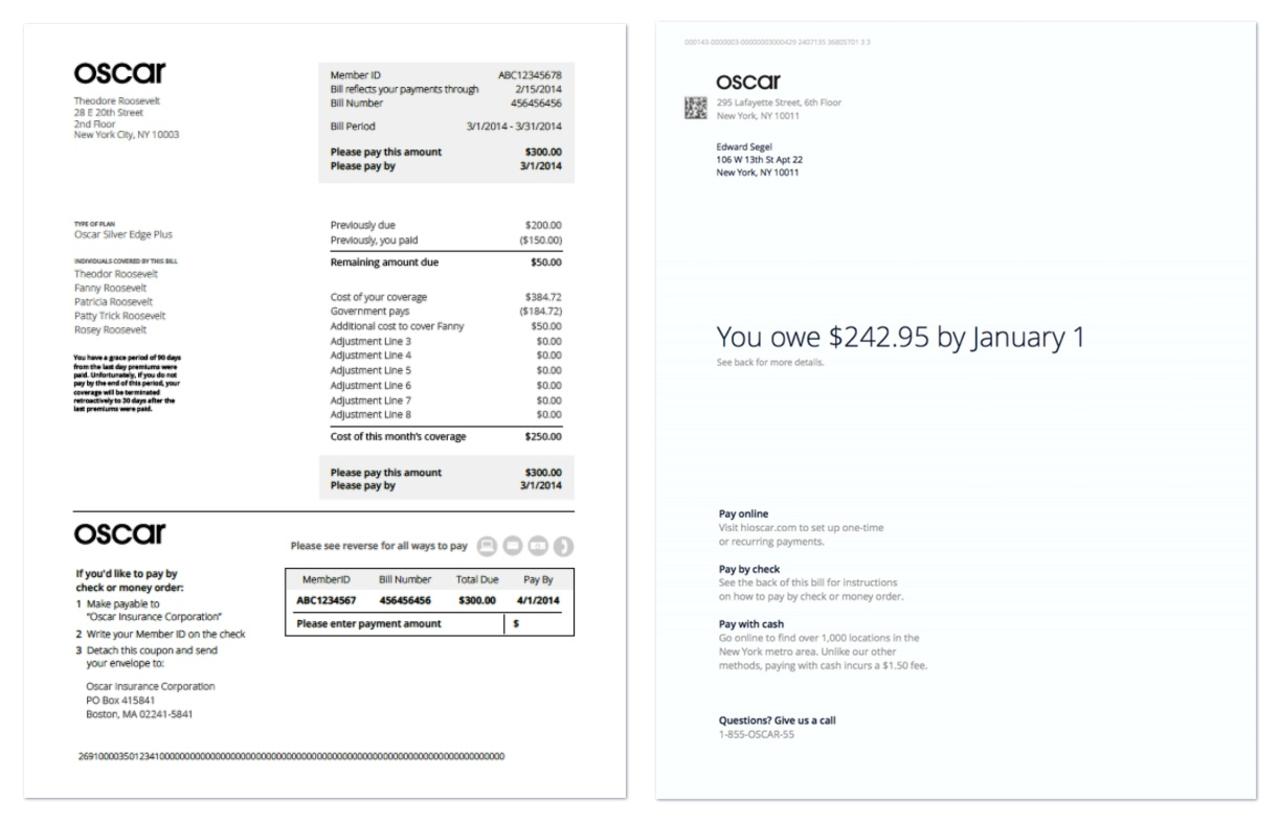
Empowered and inspired by the Affordable Care Act, which broke the link between where people work and what insurance they apply for, Oscar started targeting the 40 million people who now had to choose their own insurance. For these consumers, Oscar was a clear win. The company not only provided upfront, predictive claims information based on smart data-crunching, but also communicated it in an informal language to navigate consumers through their options and call for action. As part of their strategy, they introduced stylish cartoons to welcome users and introduce them to Oscar with a friendly tone. The consumer interface not only made it easier for customers to pick plans right for them but also provided them with the details most relevant to them e.g. below is an example of how Oscar simplified billing documents to highlight what mattered the most – the amount and date of payment.
The company’s tech base also includes complex algorithms which recognize conditions based on everyday descriptions input by consumers making the client experience even better.
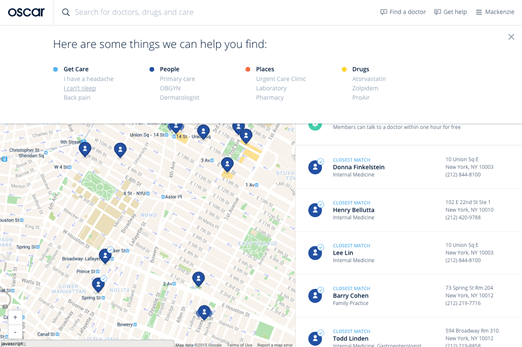
Clients use technology to evaluate the best doctors for them or even get minor illnesses treated by providers they communicate with over the internet. This can help them achieve better health outcomes while Oscar can reduce the associated cost of health care. Oscar also offers its customers incentives like cash for flu shots and money back for meeting goals specific to its partner wearable (the Misfit) that encourage users to live healthier lifestyles.
Technology:
Oscar’s key advantage is its technology platform. The platform uses established Amazon web services infrastructure and cloud technology to creatively analyze data and consistently improve. The existing big health insurance players like UnitedHealth cannot move to cloud services abruptly due to historical reliance on legacy systems, which may cost the big players a lot of money and reputation.
The foundation of Oscar’s technology is the concept of “narrow networks” – channeling business to a relatively small number of hospitals and doctors in each city in exchange for high discounts to eventually reduce the cost of healthcare. So far, Oscar has been operating at a loss – $100 million loss in 2015 – especially because it doesn’t have the narrow networks model in the two states with the highest coverage – New York and New Jersey.
Future challenges:
a. Obamacare played a vital role in creating an atmosphere where Oscar could thrive. Although new customers, acquired through Affordable Care Act, were in more need of health care than the traditional market, Oscar took upon this challenge to serve and delight this market; however, with the recent political uncertainty, Oscar’s management is concerned about the company’s future.
b. Since the company is still in negative profitability, it relies consistently on external funding to grow further. This puts pressure on their growth targets. Profitability can be improved in the future by increasing prices in selective regions and implementing the “narrow networks” concept across vast geographies such as NY and NJ.
c. Although Oscar offers an innovative health care insurance product, the company only has 140,000 members as of now vs. 27.5 million for UnitedHealth. At the same time, UnitedHealth has been known to experiment with “narrow networks” model and could potentially pose a threat to Oscar in the future. Other companies are taking Oscar’s model even further – on top of simpler customer experience, Zoom Healthcare and Harken Health run ambulatory-care facilities themselves, partly breaking down the barrier between the companies that provide health care and those that pay for it.
Sources:
https://aws.amazon.com/blogs/aws/oscar-health-a-new-kind-of-health-insurance-company-powered-by-aws/
http://www.zdnet.com/article/how-oscar-is-using-cloud-and-big-data-to-disrupt-health-insurance/
https://aws.amazon.com/solutions/case-studies/oscar-insurance/
http://www.cnbc.com/2016/06/16/oscar-may-be-obamacares-biggest-casualty.html
http://firstround.com/review/Simple-Design-is-What-You-Need-Not-What-You-Want-1/