Healthcare Goes Digital: Allscripts Moves to Electronic Health Records

The U.S. healthcare system is in the midst of a major reform, with a focus on reducing healthcare spend while maintaining quality of care. One aspect of this is the move to digital patient records. Electronic Health Records (EHRs) intend to improve information sharing across points of care, to improve efficiency across the system.
US healthcare reform: An opportunity for digitization
In 2008, healthcare spend in the United States was estimated at $3.2 trillion, higher than the spend in “Japan, Germany, France, China, the U.K., Italy, Canada, Brazil, Spain and Australia combined.”[1] In response, the Obama administration launched a healthcare reform with two main goals: Increase access to and quality of care, and reduce healthcare cost. One component of the reform was improving information-sharing across providers. This is where Electronic Health Records (EHRs)– a digitized version of a patient’s paper chart – came into play. The government invested $40 Billion in IT and provided financial incentives as well as penalized for failing to move to electronic records by 2016[2] (see Exhibit 1 for roll-out volumes).
Exhibit 1: EHR adoption rates [8]

However, EHRs required new IT platforms, which is where Allscripts saw its opportunity. Prior to 2007, Allscripts provided practice management tools to healthcare providers[4]. When the government mandated EHRs, Allscripts made a strategic move into the digital space to support providers in a timely implementation of the government mandate. Since then, Allscripts has become a major player in the digital world of healthcare, providing an entire suite of digital services (e.g., EHRs, financial management), ranking amongst the top providers of EHR software[3] and engaging 7.2 million patients on their EHR platform.[4]
The situation outlined above presents a unique example of the dynamics of digitization at play: The government mandated providers to move to EHRs as part of the healthcare reform. Yet, providers lacked the necessary IT infrastructure to do so. This created an opportunity for private companies in the field to focus on EHR platforms, and thus partner with healthcare providers in this process of digitization.
At this point, it is worth examining how the digitization of health records adds value across the healthcare value chain:
- Increased transparency across points of care by allowing doctors insight into previous tests and diagnostics findings[5]
- Reduced cost due to less duplication of diagnostics, effective prescription of drugs (especially generics) and tailored treatment. These savings are significant: One study estimates that a Canadian hospital generated approximately $100,000 savings per hospital bed annually due to improved efficiency in care after adopting EHRs3, and US-wide savings across providers may amount to as much as $40 billion annually [2]
- Improved operations by linking EHRs to other digital systems such as bed-management and equipment scheduling software [2]
- Higher quality of care as providers can better communicate across points of care and and tailor treatment accordingly[6]
- Increased insight into personal health history for patients through access to EHRs [6]
This may sound like a win-win situation…yet, challenges are looming:
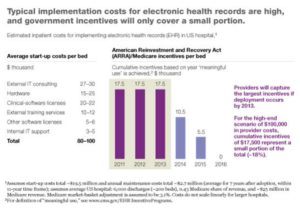
- Implementation is costly: Providers require costly IT infrastructure as well as staff training to ensure proper use of EHRs. Furthermore, government subsidies and incentives leave a significant cost to the provider (Exhibit 2).
- Proper use of EHRs is time consuming: Nurses and doctors are spending a significant amount of time each day filling out EHRs, instead of spending time with patients, leading to increased frustration and less complete data entry [5]
- Lack of standardization: In 2014, the New York Times reported that only “14 percent of physicians can exchange patient data with outside hospitals and providers”[7] This defeats the purpose of EHRs, and must be addresses in order to achieve intended goals of digitized health records.
Allscripts to the rescue: How can Allscripts –in its market leader position –improve the experience?
- Standardization across platforms is key to improve ease of use and effectiveness of EHRs. Allscripts should collaborate with other EHR providers to increase the degree of standardization across IT platforms.
- Sharing rates remain low, even for providers with the same EHR system. Allscripts services a wide network of healthcare providers, and could thus play a more active role in encouraging the sharing and active use of EHRs across points of care.
- Administrative burden is time consuming and frustrating: Allscripts could find ways to alleviate the administrative burden placed on providers. This could be done by providing dedicated support staff to help record patient conditions into the EHRs and to free up time of nurses and doctors.
US healthcare- A long road to more efficiency
The healthcare industry is faced with significant challenges and is undergoing major transformation. Technology and digitization will play a critical role in improving efficiencies. EHRs are one example of technology impacting healthcare, and it remains to be seen how the industry will leverage technology to transform over the next few years.
Exhibit 2: Implementation cost of EHRs [5]
(Word count: 790)
[1] Website: http://obamacarefacts.com/healthcare-facts/
[2] “The US Stimulus Program is Taking Medical Records Online”, McKinsey Quarterly, July 2009. McKinsey& Company.
[3] http://www.curemd.com/top-ehr-vendors/
[4] http://www.allscripts.com/allscripts-com/about-us
[5] “Reforming hospitals with IT investments”. Laflamme, F., Pietraszek, W., Rajadhyax, N.McKinsey and Company.
[6] Website source: http://www.healthit.gov/buzz-blog/electronic-health-and-medical-records/emr-vs-ehr-difference/
[7] “Doctors Find Barriers to Sharing Digital Medical Records”, Creswell, J., New York Times, 09/30/2014
[8] Website source: http://dashboard.healthit.gov/evaluations/data-briefs/non-federal-acute-care-hospital-ehr-adoption-2008-2015.php



Interesting article about a really big issue! So many problems with EHR still, even after all those billions have been spent:
-Very high fragmentation among EHR providers and lack of strong collaboration on interoperability (opening up APIs, using standardized data structures, encouraging more sharing across platforms, etc.). Trench warfare over market share means everybody loses.
-HIPAA makes any sort of innovation especially hard in healthcare IT. Say you’re trying to move healthcare data to the cloud. Well, you can’t just move it to any cloud you have to jump through a ton of hoops to make sure it’s a HIPAA-compliant cloud. A lot of it is pretty meaningless stuff. You might just be operating on an AWS box either way.
-EHR tools are mostly built for revenue cycle — they are bad at pretty much everything else (outcomes or bundled payment scenarios, for example, which appears to be where the world is going…maybe…though post-Trump who knows where the world is going).
The third challenge you raise (lack of standardization) is very interesting. Based on some research I read as part of my post (Dimitrov, D. V. Medical Internet of Things and Big Data in Healthcare. 22, 156–163 (2016).), it is clear that legacy EHRs are the root cause of some information sharing hurdles. These legacy EHRs fragment data into organizational silos. In my view the recent healthcare reform did not do enough to force the transition of old, siloed EHR systems, to more modern and open systems. EHR companies will always resist a fully open system because they want to increase the cost of switching away from their platform. I think it is the role of regulators to introduce some tension into this equation, and force a degree of openness that maximizes value for healthcare institutions, payers and patients. Your action plan to enhance standardization across institutions would be a great industry-driven step forward!
The lack of standardization with electronic health records is a major issue without a clear path forward. While it would be great for the major producers of EHR platforms to come together behind a common standard, it isn’t clear what the motivation for Allscripts (or other EHR companies) would be to take on that cost without an external stakeholder – whether regulatory or customers – pushing them to do so. However, low sharing rates between providers on the same platform seems like lower hanging fruit that could be solved with additional training that helps providers see the value EHRs provide, perhaps combined with targeting specific key decision makers that could encourage their colleagues to create a culture of information sharing.
This is really interesting, Hannah. While the amount of paper in the US healthcare system and the lack of information flowing astonishes me, I am definitely concerned about how a shift to digital will be ultimately implemented. While I think a private player has a huge opportunity ahead, I wonder if this has to be a result of a government mandate or effort – it’s like a network effect that needs to have a serious majority of people on the platform in order for the network to work.
In the UK, which has a public healthcare system, the National Health Service has faced several challenges in getting healthcare records online. In fact, the first efforts to outsource the project to CSC have cost the UK taxpayers 10Bn pounds as of 2013, to the point of which they had to shut down the project. They have made more progress since then, but it has been very challenging.
[1] https://www.theguardian.com/society/2013/sep/18/nhs-records-system-10bn