Massachusetts General Hospital: Digitizing Patient Care

Hospitals face some of the most daunting digital challenges: an unprecedented growth in unstructured data, the need to standardize IT platforms, and increases in sophisticated cyber threats. On top of that, hospitals are also facing pressure to deliver digital care.[1] Massachusetts General Hospital (MGH) has consistently been ranked among the best hospitals in the US.[2] However, although MGH has undergone digital transformations to integrate and enhance patient care, its digital acumen is lagging behind that of other top hospitals.
Integrating care through digital transformation
In 2016, MGH, along with several other Partners HealthCare hospitals, transitioned off its home-governed EMR system and implemented Epic’s EMR.[3] The aim was to have one integrated system across all Partners facilities to allow for more coordinated patient care.[4] Keith Jennings, MGH’s CIO, described a vision of “one patient, one record, one bill and hopefully the best care to our patients across the whole continuum in a very efficient or most efficient way possible”.[5] By standardizing patient data across all Partners hospitals, patients visiting different hospitals would receive more integrated care.
The transition was a huge undertaking. The system took 3 years to build and cost $1.2 billion, twice as much the initial price of $600 million. Jennings described it as a “business transformation” rather than simply an IT implementation. MGH used a staggered implementation approach, whereby Jennings’ team simultaneously kept the home-governed system running, executed data conversions, tested the new system in cycles, and trained employees on the new system.[6]
The rollout was well-received by clinicians. For instance, prior to the system’s integration, patients’ vital signs were only recorded in plastic binders (hard to imagine that in 2016, MGH still hadn’t digitalized vital signs!). With Epic’s EMR, clinicians can now view vital signs with a single click. That said, clinicians have identified some challenges with the system: too many bells and whistles that detract from easily understanding patient information, hard-coded responses that inhibit clinicians from providing customization in atypical situations, and gaps in understanding of clinical practices (e.g., it is easier to order 12 days of intravenous fluid than 12 hours’ worth).[7] It is clear that for digital transformations to be successful in the healthcare space, simplicity, flexibility, and listening to the voices of frontline users should be prioritized.
Enhancing care through digital transformation
MGH’s Healthcare Transformation Lab (HTL) was launched in April 2014 “to improve the experience and value of healthcare through collaborative innovation”. By bringing together clinicians, engineers, designers, and entrepreneurs from MGH and institutions including MIT and HBS, MGH has implemented digital transformation solutions to enhance patient engagement and improve the clinician experience.[8],[9]
Patient engagement transformations aim to equip patients with the tools to be active participants in their own health. For example, the Visit Navigator and Digital Mapping seek to improve patients’ experience navigating MGH’s campus through responsive, web-based, interactive digital maps that show everything from buildings to ATM locations around the hospital.
Clinician experience transformations aim to reduce clinicians’ administrative burden so that they can spend more time interacting with patients and less time dealing with paperwork. For example, MGH implemented highly trained scribes to address clinicians’ complaint that the use of EMR requires them to spend more time focused on the computer screen rather than on the patient. The Mass General Physicians Organization (MGPO) is now exploring ways to use virtual scribes so that more clinicians can benefit in a cost-efficient manner.[10]
Other digital initiatives have benefited both patients and clinicians:
Telemedicine
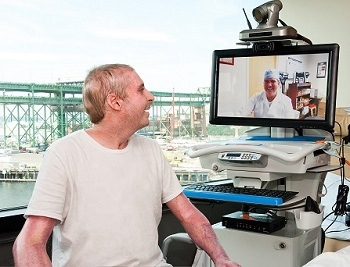
TeleHealth enables clinicians to provide high-quality care to patients virtually (usually via video-conferencing), thus improving access and convenience. TeleHealth has been implemented across various departments at MGH:
- Within pediatrics, clinicians specializing in pediatric and neonatal intensive care are using video-conferencing technology to provide medical advice to community hospitals.[11]
- The TeleBurns program allows burn patients to avoid unnecessary travel for follow-up visits and receive high-quality care from their community. According to a TeleBurns patient, “Staying in contact with my Mass General doctor from the convenience of Spaulding was huge… My virtual visit only took 20 minutes instead of a whole day of transport to Mass General”.[12]
- The TeleHeart program enables Heart Center clinicians to provide remote follow-up care to existing patients at home.[13]
- TeleNeurology offers best-in-class neurology care to 23 community hospitals and Virtual Visits to MGH patients. Over 50 neurologists have conducted more than 700 virtual visits, which has reduced follow-up visit durations by 33% (while maintaining patient satisfaction rates above 90%) and freeing up clinician time for new patients.[14]
- The TelePsychiatry program enables patients to avoid the time, cost and stress associated with traveling to the hospital by using video-conferencing.[15]
Artificial intelligence
MGH has also started to integrate AI into their care. For example, radiologists depend on high-quality diagnostic images to accurately diagnose patients but acquiring enough data to generate high-quality images comes at a cost: increased radiation (for CT and PET) or uncomfortably long scan times (for MRI). A new technique called AUTOMAP (automated transform by manifold approximation) developed at MGH uses deep learning artificial intelligence to correctly reconstruct images from imperfect raw data, thus leading to better diagnoses and improved patient outcomes.[16]
AI is also being used to better predict which high-risk breast cancer lesions should be surgically removed. Typically, among women with high-risk breast lesions (areas that look suspicious on a mammogram and have abnormal but not cancerous cells) who receive surgery, 90% of the surgeries end up being unnecessary (the lesions are benign). When tested, MGH’s algorithm correctly diagnosed 97% of 335 high-risk lesions as malignant and reduced the number of unnecessary surgeries by over 30% compared to current methods.[17] Reducing the number of unnecessary surgeries would lead to more patients with improved quality of life.
Digital transformation opportunities
Despite these changes, MGH has not adopted revolutionary technologies as quickly as other hospitals. For example, 155 hospitals and healthcare organizations are now using IBM Watson for Oncology to recommend appropriate treatments for cancer patients based on Watson’s expansive data (medical literature, guidelines, trials, articles, and patient data) and ability to understand medical records and apply natural language processing and advanced cognitive algorithms to each patient.[18],[19] Quickly being able to identify the best treatment for a cancer patient could be the difference between life or death.
Other hospitals are using AI to match patients to clinical trials. In the US, only 5% of cancer patients participate in clinical trials since the matching and enrollment process is typically done manually. This leads to low clinical trial enrollment rates, resulting in slow or discontinued trials and subsequently less access to better therapies. Other top hospitals such as the Mayo Clinic are using Watson for Clinical Trials Matching to accurately match patients to clinic trials.[20] According to Dr. Steven Alberts at the Mayo Clinic, “In an area like cancer — where time is of the essence — the speed and accuracy that Watson offers will allow us to develop an individualized treatment plan more efficiently, so we can deliver exactly the care that the patient needs”.[21] 11 months after implementing Watson in July 2016, Watson has ensured that all patients are screening for all available clinical trial opportunities, leading to an 80% increase in enrollment to Mayo’s breast cancer clinical trials.
The future of MGH
For MGH to remain competitive, it must adopt more radical transformations such as those implemented by other hospitals. From virtual reality surgical training to the use of blockchain in supply chain management, the potential for digital to transform hospitals is huge. However, such initiatives are likely to face internal resistance. Clinicians may be skeptical of the technologies’ potential or even worried about the possibility of their jobs being replaced by such technologies. Administrators may question the value of implementing such expensive technologies (MD Anderson spent over $62 million to implement Watson, only to back out before completion)[22], especially given questions on how to get reimbursed for these new products.
The greatest barrier to implementing such technologies is not the implementation of the technology itself but getting buy-in from the people involved. The first step is to create a culture of digital transformation, whereby senior management drives support for its implementation and the voices of frontline workers are heard. The voices of the most vocal opponents should also be heard, since they may even begin to take pride in driving this transformation.[23] Such technologies must also be able to communicate with existing and future applications, devices, and technologies. They must therefore be implemented in a way that offers flexibility and scalability. Finally, hospitals should continue to develop employees’ digital competence and support their transition.[24] By communicating and demonstrating the value of the new technology to end users, hospitals like MGH can begin to get more buy-in to ultimately deliver better care.
Sources
[1] https://www.usa.philips.com/healthcare/nobounds/phoenix-childrens-digital-healthcare-transformation#_continue-reading
[2] https://www.flipsnack.com/HTL2014/annual-report-2015-2016.html
[3] https://searchhealthit.techtarget.com/video/Epics-EHR-Challenges-and-lessons-learned-at-Mass-General
[4] https://www.bostonglobe.com/business/2016/04/05/epic-upgrade-mass-general/9NIikFtLwWS8rysvZOxxyH/story.html
[5] https://searchhealthit.techtarget.com/video/Epics-EHR-Challenges-and-lessons-learned-at-Mass-General
[6] https://searchhealthit.techtarget.com/video/Epics-EHR-Challenges-and-lessons-learned-at-Mass-General
[7] https://www.xconomy.com/boston/2016/05/10/mgh-goes-epic-what-i-learned-in-the-trenches/
[8] http://healthcaretransformation.org/who-we-are/
[9] https://www.massgeneral.org/News/newsarticle.aspx?id=4748
[10] https://www.flipsnack.com/HTL2014/annual-report-2015-2016.html
[11] https://www.massgeneral.org/children/telehealth/default.aspx
[12] https://www.massgeneral.org/telehealth/teleburns.aspx
[13] https://www.massgeneral.org/telehealth/teleheart.aspx
[14] https://www.massgeneral.org/teleneurology/overview/
[15] https://www.massgeneral.org/telehealth/telepsychiatry.aspx
[16] https://www.massgeneral.org/News/pressrelease.aspx?id=2229
[17] https://www.massgeneral.org/psychiatry/news/newsarticle.aspx?id=6543
[18] https://www.ibm.com/watson/health/oncology-and-genomics/oncology/
[19] https://www.fool.com/investing/2018/01/12/4-ways-ibm-watsons-artificial-intelligence-is-chan.aspx
[20] http://www.healthcareitnews.com/news/mayo-clinic-boosts-clinical-trials-ibm-watson-artificial-intelligence
[21] https://www.mayoclinic.org/giving-to-mayo-clinic/philanthropy-in-action/features-stories/artificial-intelligence-gets-real
[22] https://www.forbes.com/sites/matthewherper/2017/02/19/md-anderson-benches-ibm-watson-in-setback-for-artificial-intelligence-in-medicine/#589b963e3774
[23] https://www.elsevier.com/connect/3-tips-on-managing-change-in-a-hospitals-digital-transformation
[24] https://www2.deloitte.com/us/en/pages/life-sciences-and-health-care/articles/global-digital-hospital-of-the-future.html





Thank you for a fascinating post! I am completely on-board with the ideas and options you mention about how new technologies can be used to improve the delivery of quality healthcare at MGH and improve the patient experience overall. However, in the challenges MGH will face, I think one factor needs to be called out even more – reimbursement. You briefly mentioned how MD Anderson backed out of the IBM Watson deal because of reimbursement concerns – I think that such lack of reimbursement for trying new, technological interventions to improve the patient experience is all too common. It is not that the payors don’t want to encourage innovation – they just want to see how it will improve their financials, and chances are that their financials will improve many years later once the technology is more mature and effectively used. Therefore, in the near term, it is more like an upfront cash burn that most payors are unwilling to undertake.
I think the key is to basically find alternate sources of capital for a provider (system) – like an innovation fund – that can be used to invest in new technologies that by definition have longer RoI periods than needed by payors. What do you think?
Ai in health will improve everything. Health will become cheaper and more accessible.
Very nice and interesting article!